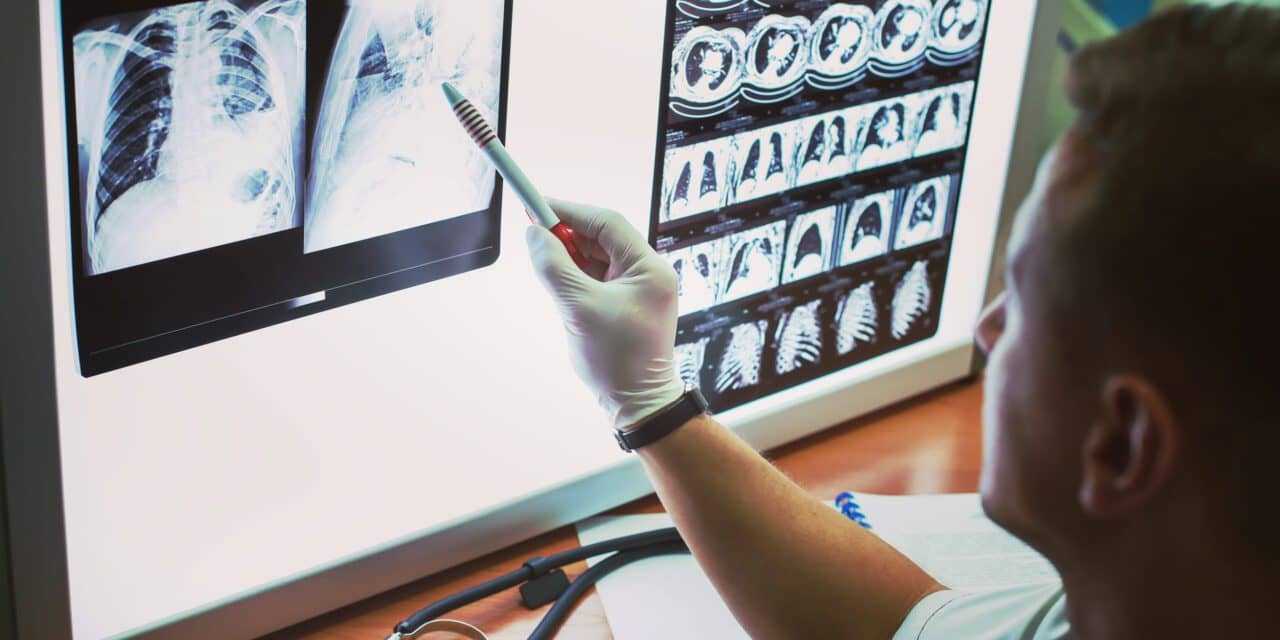
Sarah had smoked a pack a day for 25 years before finally quitting five years ago. At 62, she met every criterion for lung cancer screening, but she’d never heard of it. Neither had her doctor mentioned it during her last physical. Sarah’s story isn’t unique. It’s the reality for millions of Americans who could benefit from a simple, potentially life-saving screening test.
Recent research from the American Cancer Society has revealed a sobering truth: only about one in five eligible individuals in the United States received lung cancer screening in 2025.
That’s just 19% of the nearly 13 million Americans who qualify for this critical preventive test.
And you know what is even more heartbreaking?
If screening rates reached 100%, an estimated 62,110 lung cancer deaths could be prevented over five years, three times more than we’re currently saving.
The Stakes Couldn’t Be Higher
Lung cancer isn’t just another health statistic; it’s personal. It’s someone’s parent, partner, or best friend. Around 225,000 new cases are diagnosed each year, with 125,000 deaths annually, making it the leading cause of cancer death in America.
Yet, unlike breast cancer or colon cancer, where screening has become part of our cultural vocabulary, lung cancer screening remains largely unknown.
The irony is painful: we have the technology to catch this deadly disease early, dramatically improving survival rates, but we’re failing to use it. When lung cancer is caught early through screening, patients often need only minimally invasive surgery, no chemotherapy, no radiation. But without screening, most cases aren’t discovered until they’ve already spread, when survival rates plummet.
So What’s Exactly Going Wrong?
The barriers keeping people from getting screened are as complex as they are frustrating. Let’s break down what’s really happening.
Nobody’s Talking About It
Perhaps the biggest obstacle is shockingly simple: most people have never heard of lung cancer screening. Studies show that 24% of eligible patients weren’t even aware they qualified for CT screening. Unlike mammograms or colonoscopies that have become household terms after decades of public awareness campaigns, lung cancer screening remains in the shadows.
Even more concerning, knowledge and fear are two major barriers, and many primary care providers aren’t consistently having conversations about screening with eligible patients. When your doctor doesn’t bring it up, how are you supposed to know you need it?
The Criteria Are Confusing
Try explaining to someone that they need screening only if they’re between 50 and 80, have smoked a lot for at least 20 years, and still smoke or quit sometime in the last 15 years. Sounds simple… until you actually say it out loud. Most people’s eyes glaze over. What’s a pack-year anyway? How do you even calculate that?
Unlike age-based screenings for other cancers that apply to broad populations, lung cancer screening has complicated eligibility requirements based on smoking history. This complexity creates confusion for both patients and healthcare providers. Some people who should be screened slip through the cracks, while others who could benefit from screening don’t meet the narrow criteria.
Fear and Stigma Run Deep
Here’s something that doesn’t show up in statistics but echoes through every lung cancer screening clinic: shame. Research found that 30% of eligible patients didn’t want to know if they had cancer. Many former and current smokers carry guilt about their smoking history, making them reluctant to seek care.
The stigma associated with smoking-related disease means patients worry about blame rather than focusing on early detection and treatment. They’re afraid of judgment from healthcare providers or worry that they’ll be lectured about choices they made decades ago. This fear keeps people away from a test that could save their lives.
It Feels Unnecessary When You Feel Fine
The most common barrier reported by eligible patients was the absence of symptoms, cited by 38%. This makes intuitive sense, but misses the entire point of screening. When you feel healthy, why would you get a test for a disease you don’t think you have?
The cruel reality of lung cancer is that symptoms rarely appear until the disease has already advanced. By the time someone develops a persistent cough, chest pain, or shortness of breath, treatment options become far more limited. Screening exists precisely to find cancer before symptoms develop, when it’s most treatable.
Access Isn’t Equal
Beyond awareness and willingness, real-world barriers prevent many eligible individuals from getting screened. Not everyone lives near a facility that offers low-dose CT scans. Taking time off work for medical appointments isn’t feasible for everyone. Getting from one place to another isn’t always easy, especially in rural areas where transportation options are limited.
Insurance coverage, while generally available, isn’t universally understood. Many people worry about costs even when screening is covered. Studies show that having insurance significantly increases screening rates, with those having private plans being much more likely to be screened.
Racial and socioeconomic disparities compound these issues. Research has consistently shown that Black smokers have lower screening rates than white smokers, contributing to worse outcomes in communities that already face health inequities.
The Screening Gap Compared to Other Cancers
Perhaps the most striking indicator that something is fundamentally wrong comes from comparing lung cancer screening to other cancer screenings. While only 17-18% of eligible individuals received lung cancer screening, 65% received breast and colorectal cancer screening, nearly four times higher.
This massive disparity demolishes the theory that people eligible for lung cancer screening simply avoid preventive healthcare. The same individuals who get their colonoscopies and mammograms aren’t getting lung cancer screening, not because they’re against preventive care, but because of systemic failures in awareness, access, and advocacy.
The Cost of Inaction Is Measured in Lives
Let’s put real numbers to the human cost of these low screening rates. At current screening uptake, only about 14,970 deaths are prevented and 190,030 life-years are gained, just a quarter of what could be achieved. That means roughly 47,000 people who could have been saved will die from lung cancer because they never got screened.
These aren’t just statistics. They’re teachers, parents, grandparents, friends, people with families who love them, with dreams they haven’t fulfilled, with grandchildren they won’t get to watch grow up. Each preventable death represents immeasurable loss, not just for the individual but for everyone connected to them.
What Would It Take to Change This?
Fixing the lung cancer screening crisis requires action at every level, from national policy to individual doctor-patient conversations.
Healthcare providers need to step up. Primary care physicians should systematically identify eligible patients and have screening conversations during annual visits. These discussions should alleviate fear and address stigma, making clear there’s no blame involved in the screening process.
Public awareness campaigns are essential. If we could make “get your annual lung screening” as common as “schedule your mammogram,” screening rates would soar. Major health organizations and cancer advocacy groups need to invest in education that reaches people where they are, through social media, community programs, and trusted local voices.
Access barriers must be removed. This means expanding screening facilities in underserved areas, ensuring insurance coverage is comprehensive and clearly communicated, and reducing financial burdens for patients. Mobile screening programs have shown promise in reaching rural and underserved communities.
Eligibility criteria might need rethinking. Recent research suggests that current guidelines miss many people who develop lung cancer, particularly women and never-smokers. Some experts now advocate for universal age-based screening similar to what we do for other cancers, which could detect far more cases while remaining cost-effective.
And if I would sum it up, and you’ve smoked heavily at any point in your life, talk to your doctor about whether lung cancer screening is right for you. If you’re a healthcare provider, make screening discussions part of your routine care for eligible patients. If you’re a policymaker or health system leader, invest in the awareness campaigns and access infrastructure needed to reach more people.
The technology exists. The evidence is clear. Low-dose CT screening saves lives. Around 70% of lung cancers detected through screening are found at early stages, compared to roughly 20% without screening. What we lack isn’t the capability to detect lung cancer early; we lack the will to ensure everyone who needs screening actually gets it.
Every person who develops late-stage lung cancer when early detection was possible represents a failure of our healthcare system. We can do better. We must do better. Because behind every screening statistic is a human being, someone who deserves every chance at a long, healthy life.
The question isn’t whether we can save more lives. We know we can. The question is whether we will.