Sarah thought it was just stress from her new job. The cramping, the urgent trips to the bathroom, the exhaustion that seemed to settle into her bones, surely it would pass once she adjusted to her routine. But weeks turned into months, and instead of improving, her symptoms worsened. Blood in her stool became a frightening reality, and the abdominal pain grew impossible to ignore. When she finally received her diagnosis of ulcerative colitis, Sarah joined the ranks of over 900,000 Americans living with this chronic inflammatory bowel disease.
Her story isn’t unique. Across the globe, millions of people navigate the complex landscape of ulcerative colitis, a condition that remains shrouded in mystery despite decades of medical research. Today, we’re pulling back the curtain on this enigmatic disease to understand what it truly means to live with UC and how modern medicine is working to solve this chronic gut puzzle.
Understanding the Beast: What Exactly Is Ulcerative Colitis?
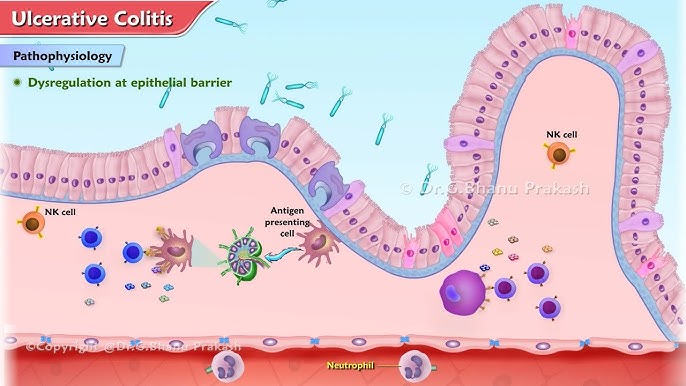
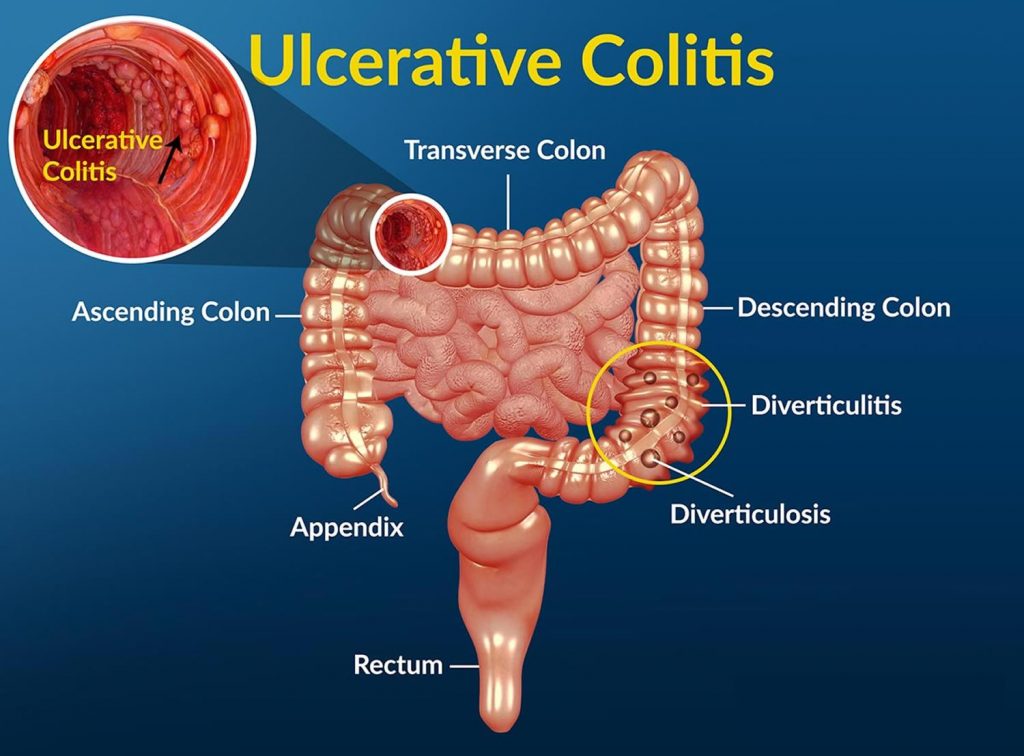
Picture your large intestine as a garden hose lined with a delicate inner layer called the mucosa. In ulcerative colitis, this lining becomes inflamed and develops painful ulcers, much like having open wounds throughout your colon and rectum. Unlike its inflammatory bowel disease cousin, Crohn’s disease, which can affect any part of the digestive tract in patches, ulcerative colitis follows a more predictable pattern—it always begins in the rectum and spreads continuously upward through the colon.
The inflammation creates a cascade of problems. The damaged intestinal lining can’t absorb nutrients properly, leading to malnutrition despite adequate food intake. The ulcers bleed, causing the telltale symptom of bloody diarrhea that often brings patients to their doctor’s office. Meanwhile, the body’s immune system, mistakenly attacking healthy tissue, creates a state of chronic inflammation that affects not just the gut, but the entire body.
What makes ulcerative colitis particularly challenging is its unpredictable nature. Patients experience periods of remission where symptoms virtually disappear, followed by flares that can range from mildly inconvenient to completely debilitating. This roller coaster existence makes it difficult for both patients and doctors to predict and manage the disease effectively.
You can read this blog also :- Caring for My Mother with Alzheimer Symptoms: 8 Ways to Cope
The Mystery of Origins: Why Does UC Develop?
Despite extensive research, the exact cause of ulcerative colitis remains elusive, like trying to solve a jigsaw puzzle with missing pieces. Scientists have identified several contributing factors, but the complete picture continues to evolve.
Genetics plays a significant role, with about 15-20% of UC patients having a family member with inflammatory bowel disease. However, having the genetic predisposition doesn’t guarantee you’ll develop the condition; it’s more like having a loaded gun that may never fire without the right triggers.
Environmental factors appear to be crucial in pulling that trigger. Our modern Western lifestyle, with its processed foods, reduced bacterial diversity, and increased antibiotic use, may be creating the perfect storm for autoimmune diseases like UC. The hygiene hypothesis suggests that our overly sanitized environments might prevent our immune systems from developing properly, leading them to attack harmless substances or even our own tissues.
Stress, both physical and emotional, can exacerbate symptoms, though it’s unlikely to cause the disease initially. Many patients report that their first flare coincided with a major life event, a death in the family, divorce, job loss, or other significant stressor. The gut-brain connection is real and powerful, with the enteric nervous system (sometimes called the “second brain”) in our intestines communicating constantly with our central nervous system.
Living with the Invisible Illness: The Human Impact
One of the most challenging aspects of ulcerative colitis is its invisible nature. Unlike a broken arm in a cast, UC symptoms aren’t obvious to others, leading to misunderstanding and sometimes skepticism from family, friends, and even employers. Patients often describe feeling isolated and frustrated when others minimize their symptoms or suggest they’re “just stressed.”
The physical symptoms extend far beyond the bathroom. Fatigue is overwhelming and constant, like trying to function with the flu every single day. Joint pain affects many patients, making simple tasks like opening jars or climbing stairs difficult. Skin problems, eye inflammation, and liver issues can all be part of the UC package, earning it the designation of a “systemic disease.”
The emotional toll is equally significant. The unpredictability of flares creates anxiety about leaving home, traveling, or participating in social activities. Many patients develop what they call “bathroom mapping”, constantly noting the location of restrooms wherever they go. This hypervigilance, while necessary for managing symptoms, can be mentally exhausting.
Relationships suffer when chronic illness enters the picture. Partners may struggle to understand the disease’s impact, while patients grapple with feelings of guilt and inadequacy. Dating becomes complicated when explaining frequent bathroom trips or dietary restrictions. Career advancement may stall when sick days accumulate or when the stress of demanding jobs triggers flares.
The Diagnostic Journey: Putting Together the Pieces
Diagnosing ulcerative colitis can be a lengthy process, often taking months or even years. The symptoms overlap with many other conditions, from irritable bowel syndrome to infections, leading to misdiagnosis and delayed treatment.
The diagnostic process typically begins with a detailed medical history and physical examination. Blood tests check for markers of inflammation, anemia from blood loss, and nutritional deficiencies. Stool samples rule out infections and parasites that could mimic UC symptoms.
The gold standard for diagnosis remains colonoscopy, though the procedure that many patients dread provides invaluable information. The scope allows doctors to directly visualize the inflamed tissue, take biopsies, and determine the extent and severity of the disease. For many patients, seeing the images of their inflamed colon provides validation that their symptoms are real and significant.
Additional imaging studies like CT scans or MRIs may be necessary to rule out complications or assess disease activity. The entire diagnostic workup can feel overwhelming, but it’s crucial for developing an effective treatment strategy.
Treatment Strategies: Fighting Back Against Inflammation
Managing ulcerative colitis requires a multifaceted approach tailored to each individual’s disease severity, extent, and response to previous treatments. The goal isn’t just to control symptoms, it’s to achieve deep remission that includes both clinical improvement and healing of the intestinal lining.
Medication forms the foundation of UC treatment. Anti-inflammatory drugs like aminosalicylates (such as mesalamine) are often the first line of defense for mild to moderate disease. These medications work directly in the colon to reduce inflammation and can be taken orally or administered as suppositories or enemas.
For more severe disease or when first-line treatments fail, immunosuppressive medications enter the picture. Corticosteroids provide rapid relief during flares but aren’t suitable for long-term use due to significant side effects. Immunomodulators like azathioprine or methotrexate work more slowly but can help maintain remission.
The treatment landscape has been revolutionized by biologic medications, sophisticated drugs that target specific components of the immune system. Medications like infliximab, adalimumab, and vedolizumab have provided hope for patients with severe, treatment-resistant disease. While expensive and requiring careful monitoring, these drugs have dramatically improved the quality of life for many UC patients.
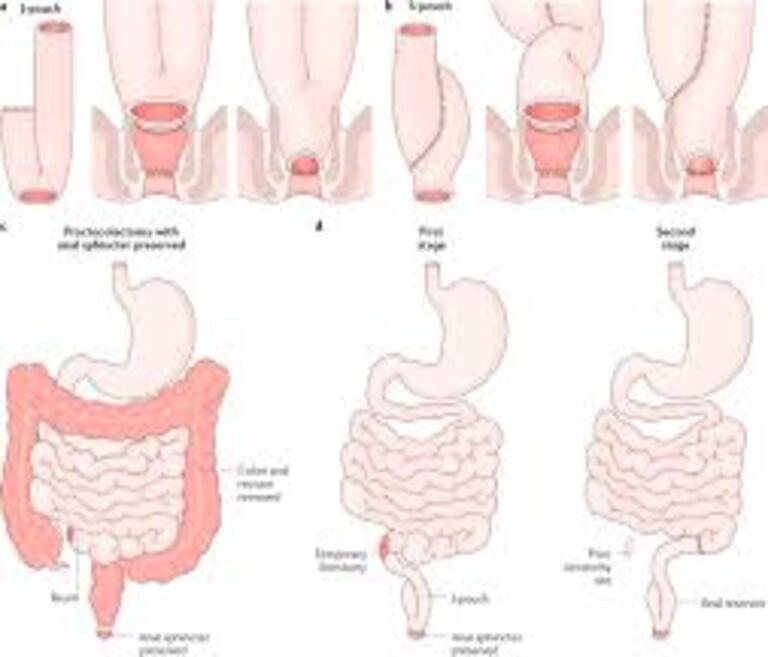
Surgery remains an option when medical therapy fails or complications develop. Unlike Crohn’s disease, UC can potentially be “cured” through removal of the entire colon and rectum, though this drastic step obviously comes with significant lifestyle changes and potential complications.
Beyond Pills: The Holistic Approach
While medication remains the cornerstone of UC treatment, many patients find that lifestyle modifications play a crucial supporting role. Diet doesn’t cause ulcerative colitis, but certain foods can trigger symptoms or worsen inflammation during flares. Common dietary triggers include spicy foods, high-fiber foods during active disease, dairy products for those with lactose intolerance, and artificial sweeteners. However, trigger foods are highly individual; what causes problems for one patient might be perfectly fine for another. Keeping a food diary can help identify personal triggers.
Stress management, while not curative, can significantly impact symptom severity. Techniques like meditation, yoga, regular exercise, and adequate sleep all contribute to overall well-being and may help reduce flare frequency. Some patients find that counseling or support groups provide valuable coping strategies and emotional support.
Probiotics, while not a cure, may help some patients maintain a healthy gut bacteria balance. The research is still evolving, but some studies suggest certain probiotic strains might be beneficial for UC patients, particularly in maintaining remission.
Hope on the Horizon: The Future of UC Treatment
The field of inflammatory bowel disease research is rapidly advancing, offering hope for better treatments and potentially even cures. Personalized medicine approaches are beginning to identify which patients will respond best to specific treatments, reducing the current trial-and-error approach. New drug targets are being explored, including medications that work on different inflammatory pathways or help repair damaged intestinal tissue. Fecal microbiota transplantation, while still experimental for UC, shows promise in restoring a healthy gut bacteria balance.
Gene therapy and stem cell treatments remain in early research phases but represent exciting potential future options. The goal isn’t just better symptom control; researchers are working toward treatments that could actually reverse the disease process and restore normal immune function.
Living Well with UC: The Path Forward
Receiving a diagnosis of ulcerative colitis can feel overwhelming, but it’s important to remember that this condition, while chronic, is manageable. With proper medical care, lifestyle modifications, and support systems, many people with UC live full, productive lives.
The key is developing a strong partnership with healthcare providers who understand the disease and are committed to finding the right treatment approach. This often means working with gastroenterologists who specialize in inflammatory bowel diseases and have experience with the latest treatments.
Building a support network is equally important. Whether through online communities, local support groups, or organizations like the Crohn’s and Colitis Foundation, connecting with others who understand the daily challenges of UC can provide invaluable emotional support and practical advice.
Ulcerative colitis may remain an enigma in many ways, but each year brings new understanding and better treatment options. For people like Sarah and millions of others worldwide, that represents not just hope, but the promise of brighter, healthier days ahead. The chronic gut puzzle is complex, but piece by piece, we’re getting closer to solving it.