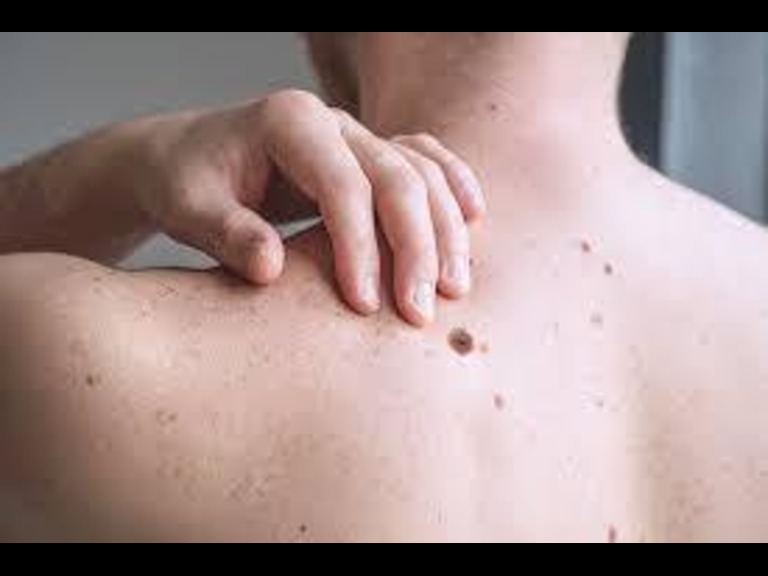
“It was just a small, dark spot on my shoulder. I almost ignored it until my daughter, a nursing student, insisted I get it checked. “That one simple choice to listen to her saved my life.”
– Sarah, melanoma survivor
If you’ve found yourself here, reading this blog, there’s a good chance that melanoma cancer has touched your life in some way. Maybe you’ve noticed a strange mole. Maybe someone close to you has received a diagnosis. Or maybe you’re just trying to understand what this disease is and how to prevent it.
Whatever your reason, know this: you’re not alone. Melanoma cancer is more than a diagnosis; it’s a deeply human experience. It affects families, friendships, routines, and emotions. But the good news is, there’s hope, knowledge, and a path forward.
Understanding Melanoma Cancer: What Is It, Really?
Let’s break this down in human terms.
Melanoma cancer begins in cells called melanocytes, the cells that give your skin its color. While other types of skin cancer often stay put, melanoma is different. It’s aggressive and unpredictable. It has the potential to spread to other parts of the body through the lymphatic system or bloodstream.
This is what makes early detection so critical.
“My dermatologist told me to think of melanoma as seeds; if you catch it before it spreads, you can stop it from growing in the wrong places,” Sarah explains.
It’s important to know: melanoma can appear anywhere, even in places that never see the sun, like your scalp, under your nails, between your toes, or the soles of your feet.
What Triggers Melanoma Cancer?
Like many health conditions, there isn’t just one cause, but several factors increase your risk.
UV Exposure: The Double-Edged Sword
We love the sun for the warmth, the light, and the joy it brings. However, the ultraviolet (UV) rays from the sun are a major trigger for melanoma cancer. Especially dangerous are the sunburns you had as a child; your skin remembers every single one.
“I worked construction in the Arizona sun for two decades with barely any sunscreen,” says Michael, 45, now living with Stage II melanoma. “Back then, I thought sunscreen was optional. Now I know better.”
Tanning beds also increase your risk significantly. There is no such thing as a safe tan from UV radiation.
You can read this blog also :- https://purewelltips.com/cbd-convention/
Genetics: When It Runs in the Family
If someone in your immediate family has had melanoma cancer, your risk may be higher. Some families carry specific gene mutations, like CDKN2A, that can make you more susceptible. Lisa, whose mother had melanoma cancer, later discovered that she carried the same gene. At first, it scared me,” she shares. “But now I see it as a gift, I stay on top of my checkups and live more aware.”
Your Unique Skin Type
Fair-skinned individuals, redheads, and people with light eyes are more vulnerable. But melanoma cancer can affect anyone, regardless of skin color.
People with darker skin are more likely to get acral lentiginous melanoma, which often appears on the palms, soles, or under the nails, places people rarely check.
How to Recognize Melanoma: The ABCDE Rule
Knowing the signs can make all the difference. Dermatologists often use the ABCDEs of melanoma:
A – Asymmetry: One half of the mole does not match the other.
B – Border: The edges are irregular, ragged, or blurred.
C – Color: Includes different shades or unexpected colors (red, white, blue).
D – Diameter: Larger than a pencil eraser (6 mm), though smaller melanomas can still be dangerous.
E – Evolving: Any change in size, shape, color, or symptoms like bleeding or itching.
“It was the itch that got me,” recalls Jake, a surfer. “This tiny spot on my back itched constantly. I almost ignored it, but my girlfriend pushed me to get it looked at. It turned out to be melanoma.”
Other Warning Signs of Melanoma Cancer
Some signs don’t follow the ABCDEs:
- A mole that appears different from all the others (the “ugly duckling” sign).
- A sore that doesn’t heal
- A mole that starts to bleed or crust
- Tingling or burning in a spot on your skin
If anything feels off, it’s worth a professional checkup.
Prevention: What You Can Actually Do
You can’t change your genes, but you can reduce other risks significantly.
Daily Sun Protection
Wear broad-spectrum SPF 30 or higher, every day, even when it’s cloudy. Reapply every 2 hours when outdoors. Sun damage accumulates over time.
“I treat sunscreen like my morning coffee, I don’t leave home without it,” says Maria, a teacher in Phoenix.
Shade and Clothing
Try to stay out of direct sunlight between 10 AM and 4 PM, when the sun’s rays are the strongest. Wear wide-brimmed hats, sunglasses, and protective clothing when outdoors.
Monthly Self-Exams
Make it a monthly habit to check your skin from head to toe. Use a mirror to help, and don’t miss those easy-to-overlook spots like your scalp, between your fingers and toes, and under your nails.
Take photos of moles you’re watching to track changes over time.
Talk to Your Doctor About Risk
If you have a family history or multiple risk factors, ask about regular dermatologist checkups, especially if you’re in a high-risk category.
Treatment Options: What Happens After Diagnosis?
Getting a melanoma cancer diagnosis is overwhelming, but you’re not powerless.
1. Surgery
For most early-stage melanomas, surgery is the first step. The goal is to remove the cancer with a clear margin of healthy tissue. It’s often done under local anesthesia.
“It was done in a single visit,” recalls Tom, a survivor. “The scar’s small. The peace of mind is huge.”
2. Immunotherapy
This treatment boosts your immune system’s ability to recognize and attack melanoma cells. It’s especially effective for later stages.
3. Targeted Therapy
If your cancer has a specific gene mutation (like BRAF), there are medications that “target” and shut down those cancer cells specifically.
4. Radiation or Chemotherapy
Less common for melanoma today, but still used in some advanced cases or when other treatments aren’t suitable.
Emotional Healing: It’s Not Just About the Skin
The emotional toll of melanoma cancer is real. Anxiety, fear, and grief are part of the journey. It’s okay to ask for help.
“I joined a support group,” shares Jennifer, diagnosed at 34. “It helped me feel less alone. I needed people who understood what I was going through.”
Counseling, talking with survivors, or simply leaning on loved ones can make a big difference in how you heal.
Inspiring Stories of Survival and Strength
Every year, thousands of people not only survive melanoma, but they thrive.
David, now five years cancer-free, reflects:
“Melanoma gave me perspective. I stopped sweating the small stuff. Now I wear sunscreen, sure. But more importantly, I live more consciously.”
Common Questions About Melanoma Cancer
Can I die from melanoma cancer?
If caught early, melanoma has a very high survival rate. That’s why awareness and skin checks are life-saving.
Should people with dark skin worry about melanoma?
Yes. Though less common, melanoma can affect anyone. People with darker skin may be more likely to develop melanoma in less sun-exposed areas, which makes it harder to detect early.
Can melanoma come back?
Yes, recurrence is possible. That’s why regular follow-ups with your dermatologist are crucial — even after successful treatment.
Is sunscreen enough?
Sunscreen is critical, but it’s just one part. Wearing protective clothing, avoiding tanning beds, and doing self-exams are equally important.
Final Thoughts: Hope is Real
Melanoma cancer can be frightening, but knowledge is powerful. Awareness leads to early detection, which leads to survival.
This isn’t just a skin condition. It’s a wake-up call to take better care of yourself and your loved ones. Whether you’re here out of concern, curiosity, or as a survivor, you’re part of a community that supports, educates, and heals together.
Your action today, checking your skin, booking an appointment, or sharing this article, might save a life. Maybe even your own.